Diabetic peripheral neuropathy: what you need to know now
Numbness, tingling, or burning in the feet can be more than a nuisance — for people with diabetes it often signals diabetic peripheral neuropathy (DPN). Catching DPN early makes a real difference: simple steps can slow damage, reduce pain, and prevent ulcers or amputations.
DPN is nerve damage caused by long-term high blood sugar and poor circulation. It usually affects the longest nerves first, so symptoms start in the toes and move upward. Common warning signs include numbness, pins-and-needles, sharp or burning pain, loss of balance, and trouble feeling temperature or pressure.
Common Symptoms and When to See a Doctor
Watch for these clear signs: constant numbness in one or both feet, pain that wakes you at night, cuts or blisters you don’t feel, or a change in walking. If you have any of those, see your healthcare provider. Also get immediate care for red, warm, or draining wounds — infections spread fast when sensation is reduced.
Your doctor will check your feet, test vibration and reflexes, and may order blood tests, nerve conduction studies, or imaging to rule out other causes. Tight blood sugar control is often the first step in any treatment plan.
Practical Treatment and Self-Care Tips
Start with blood sugar control and foot care. Keep blood glucose in your target range, trim nails carefully, moisturize dry skin (but not between toes), and wear supportive, well-fitting shoes. Inspect your feet daily with a mirror or ask someone to help.
For pain, common medicines include gabapentin and pregabalin, duloxetine, and some tricyclic antidepressants. Topical options like capsaicin cream or lidocaine patches help some people. Discuss side effects and dosing with your clinician — not every drug fits every patient.
Non-drug approaches can work too: regular low-impact exercise improves circulation and balance, physical therapy can reduce falls, and mindfulness or cognitive behavioral therapy helps with chronic pain. For certain cases, procedures like nerve blocks or referral to a pain specialist may be useful.
Protect your feet: never walk barefoot, check shoes for debris, avoid extreme temperatures, and quit smoking to improve blood flow. If you notice slow-healing sores, swelling, or changing skin color, get urgent medical evaluation.
Supplements like alpha-lipoic acid and B vitamins show some benefit for nerve symptoms in studies, but results vary. Tell your provider about any supplements to avoid interactions with medications.
Preventing DPN starts with daily habits: consistent blood sugar checks, healthy meals, regular activity, and regular foot exams by a clinician. Small, steady changes reduce risk more than short bursts of effort.
If you have diabetes and new foot symptoms, don’t ignore them. Early action gives you the best chance to keep feeling steady and avoid complications.
Talk to your team about regular foot exams, medication reviews, and referrals to podiatry or neurology if pain or numbness worsens. Many clinics offer diabetic foot services and nurse-led wound care to speed healing. Keep a symptom diary — dates, pain level, new wounds — to help your clinician spot trends.
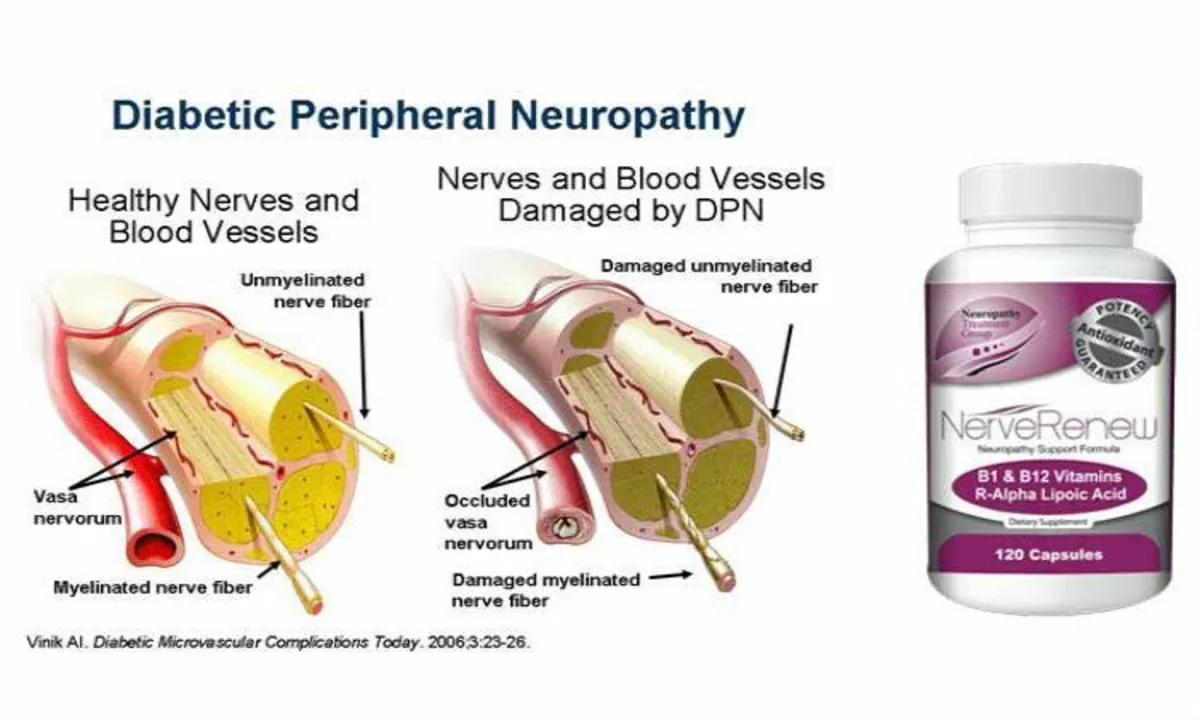
Diabetic Peripheral Neuropathy and Vision Loss: What You Need to Know
As a diabetic, I've been learning about the risks of diabetic peripheral neuropathy and vision loss. In just five sentences, here's what you need to know: Diabetic peripheral neuropathy is a common complication of diabetes, affecting the nerves in our legs and feet, leading to pain and numbness. This condition can also cause vision loss if it affects the nerves in our eyes. It's essential to manage our blood sugar levels and have regular check-ups with our healthcare providers to prevent these complications. Early detection and treatment can help reduce the risk of severe consequences. Remember, staying informed and proactive about our health is the key to living a better life with diabetes.
Read More



