Bariatric Surgery: What to Expect, Risks, and Recovery
Bariatric surgery isn't a quick fix. It changes how your body handles food and can cut serious health risks tied to obesity. If you’re thinking about surgery, you need clear steps, real risks, and a realistic recovery plan. This page lays out what to expect before, during, and after surgery so you can make a smarter choice.
Who is a good candidate? Most centers consider surgery when BMI is 40 or higher, or 35 with obesity-related conditions like type 2 diabetes, sleep apnea, or severe joint pain. Age, previous surgeries, and mental health are part of the decision too. Expect screening that includes blood work, heart and lung checks, a nutrition plan, and a psychological evaluation — teams want to make sure you’re ready for lifelong changes.
Common procedures and how they differ
Different operations suit different needs. The most common are:
- Roux-en-Y gastric bypass: reduces stomach size and reroutes part of the small intestine. Strong weight loss but higher risk of nutritional deficiencies.
- Sleeve gastrectomy: removes part of the stomach to reduce hunger and intake. Simpler than bypass and very common.
- Adjustable gastric band: places a band around the stomach to limit food. Less invasive but lower long-term success for many people.
- Biliopancreatic diversion with duodenal switch: a larger surgery that combines stomach reduction and major absorption changes. Usually reserved for very high BMI or specific medical reasons.
Preparation, medications, and realistic recovery
Preparation matters. Surgeons often require a pre-op weight loss plan, stop-smoking support, and sometimes liver-shrinking diets. Tell your team about every drug and supplement you take. Some meds need to stop before surgery (like certain blood thinners), and many prescriptions change after surgery because absorption shifts.
After surgery, expect a staged diet: clear liquids for days, then purees, then soft foods, and finally regular foods over weeks. Hospital stays are usually 1–3 days for sleeve or bypass, with most people back to light activity in 2–4 weeks and more intense exercise allowed around 6–8 weeks depending on your surgeon's advice.
Long-term care is crucial. You’ll likely need daily vitamins — B12, iron, calcium, and vitamin D are common — and regular lab checks every few months the first year. Watch for red flags like severe abdominal pain, high fever, persistent vomiting, or signs of dehydration. These need urgent care.
Picking a surgeon and a center with experience matters more than price. Ask about complication rates, follow-up support, and access to nutritionists and mental health care. Join a support group and set realistic goals: weight loss improves health, but it takes effort and lifelong habit changes.
If you have questions about medication changes after bariatric surgery or want reliable drug info, check resources on RxStore-365 or talk with your pharmacist and surgical team before you decide.
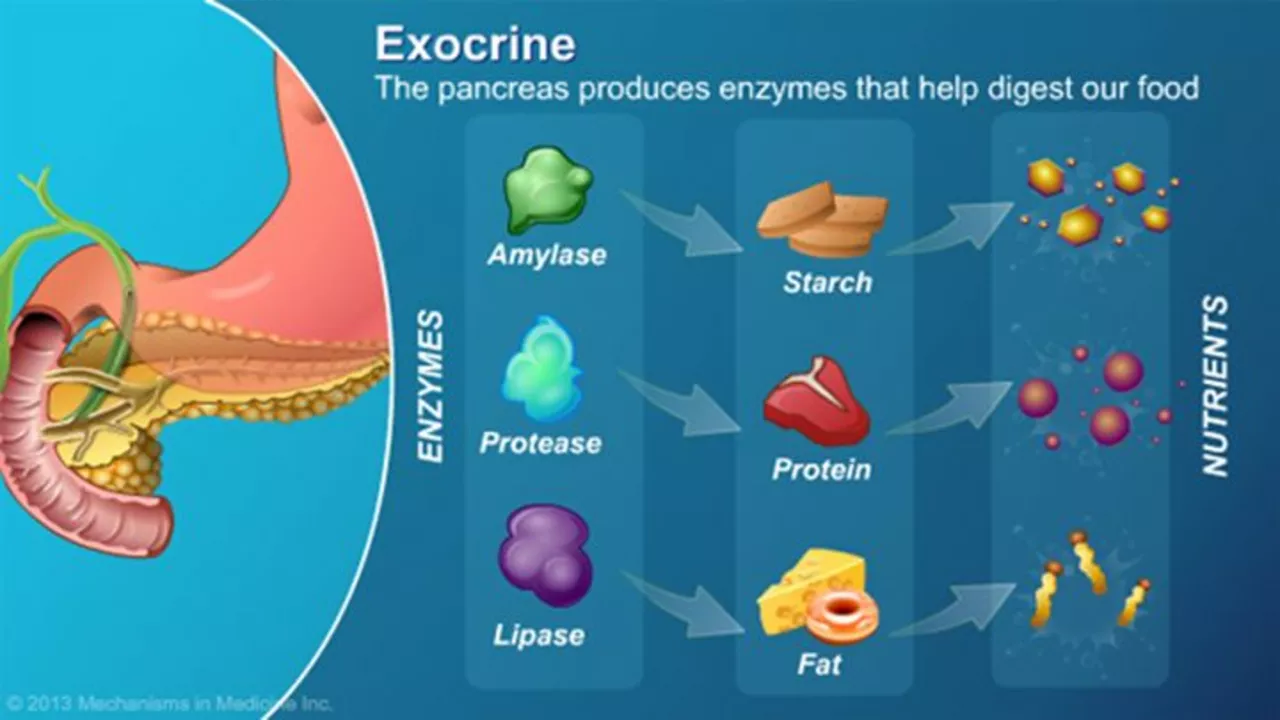
Pancrelipase and Bariatric Surgery: What You Need to Know
As a blogger, I recently came across the topic of Pancrelipase and Bariatric surgery and felt the need to share some important information with my readers. Pancrelipase is an essential enzyme supplement that helps in the digestion of fats, proteins, and carbohydrates, particularly in patients who have undergone bariatric surgery. Bariatric surgery is a procedure that helps in weight loss by altering the digestive system, often leading to a decreased ability to absorb nutrients. It's crucial for patients to understand the importance of taking Pancrelipase supplements post-surgery to maintain proper nutrition and avoid potential complications. So, if you or someone you know has undergone bariatric surgery, make sure to discuss Pancrelipase with your healthcare provider to ensure optimal recovery and well-being.
Read More