Vision Loss: What to Watch For and How Medications Can Matter
Sudden or progressive loss of sight is scary and often time-sensitive. Some causes are urgent — like a detached retina or stroke — while others build slowly, such as diabetic damage or medication effects. This page gives clear, practical steps you can take right away, how to spot warning signs, and which drugs are worth asking your doctor about.
Quick warning signs
If any of these happen, stop what you’re doing and get medical help now: sudden loss of vision in one or both eyes, big increase in floaters or flashes of light, a curtain or shadow across part of your view, severe eye pain with redness, or sudden double vision. Don’t wait for an appointment next week — fast evaluation can save sight.
Less urgent but still important: steady blurring, trouble reading, increased glare at night, or new blind spots that appear over weeks to months. Book an eye exam and bring a list of every medicine, supplement, and topical product you use.
Medications that can affect vision
Many drugs help us, but some carry eye risks. Here are common examples to discuss with your provider:
- Hydroxychloroquine: long-term use can cause retinal damage; routine eye checks are usually recommended.
- Isotretinoin and similar vitamin A derivatives: can cause dry eyes, night vision changes, and rarely more serious problems.
- Topiramate: known to trigger sudden angle-closure glaucoma in some people, causing pain and blurred vision.
- Vigabatrin: can cause permanent peripheral vision loss; vision monitoring is standard while taking it.
- Steroids (oral or injected): increase risk of cataracts and glaucoma with prolonged use.
These are examples, not a complete list. If you or a family member notices new vision problems after starting a drug, report it immediately. Your prescriber can weigh risks, change the dose, or switch medications.
Want to check interactions or side effects? Use trusted resources, talk to a pharmacist, or ask an eye specialist. Keep one up-to-date medication list and share it at every appointment.
Prevention matters. Control chronic conditions that harm eyes: keep blood sugar and blood pressure in target ranges, stop smoking, wear sunglasses outside, and schedule regular eye exams — especially if you take medications with known eye risks.
Finally, know what to do in the moment: don’t drive if your vision is affected, avoid eye rubbing, and seek urgent care for sudden changes. Quick action and good communication with your healthcare team are the fastest way to protect your sight.
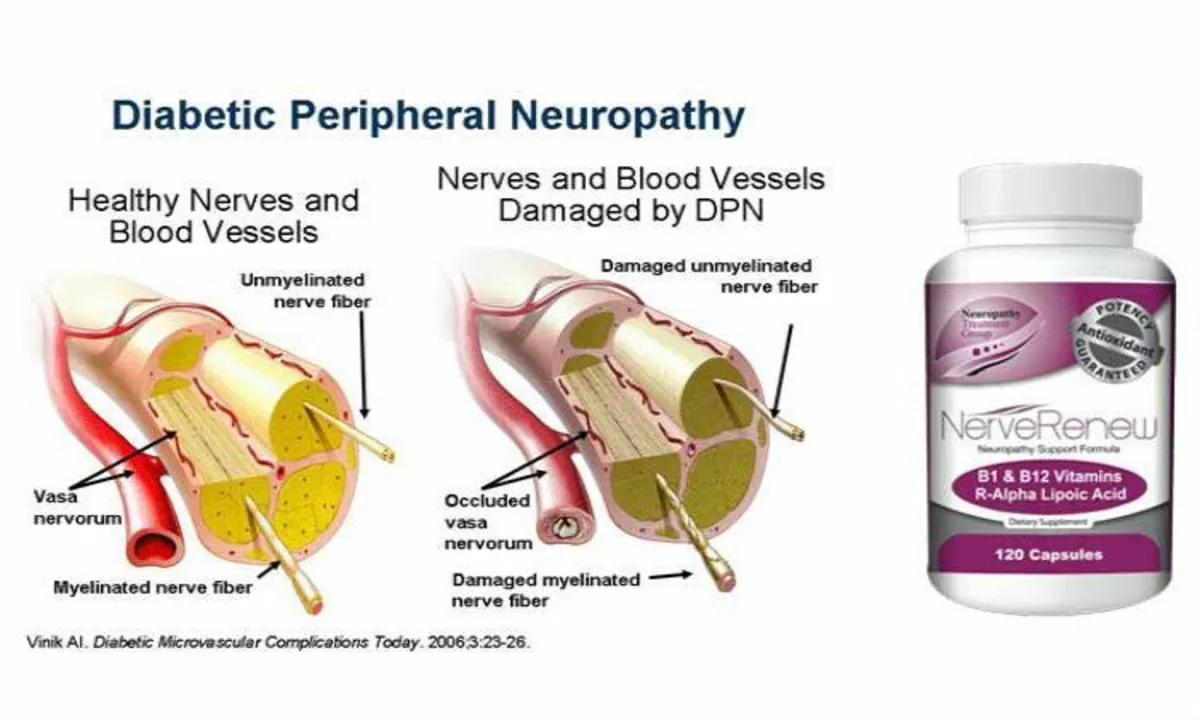
Diabetic Peripheral Neuropathy and Vision Loss: What You Need to Know
As a diabetic, I've been learning about the risks of diabetic peripheral neuropathy and vision loss. In just five sentences, here's what you need to know: Diabetic peripheral neuropathy is a common complication of diabetes, affecting the nerves in our legs and feet, leading to pain and numbness. This condition can also cause vision loss if it affects the nerves in our eyes. It's essential to manage our blood sugar levels and have regular check-ups with our healthcare providers to prevent these complications. Early detection and treatment can help reduce the risk of severe consequences. Remember, staying informed and proactive about our health is the key to living a better life with diabetes.
Read More



