Heart Attacks: Recognize, React, Recover
A heart attack can happen fast. Knowing the signs and what to do in the first few minutes can save a life. This page gives clear, practical steps you can use right away: how to spot a heart attack, what to do before help arrives, and what recovery usually looks like.
Recognize the signs
Classic chest pain is common, but a heart attack can look different. Watch for pressure, squeezing, or a heavy feeling in the center of the chest that lasts more than a few minutes. Pain may move to the jaw, neck, shoulder, or left arm. Shortness of breath, cold sweat, lightheadedness, nausea, or sudden fatigue are also red flags—especially in women and older adults, who sometimes have less obvious symptoms.
If you or someone else shows these signs, call emergency services immediately. Don’t drive yourself to the hospital unless there's no other option. If the person is conscious and not allergic, chewing one regular-strength aspirin can slow clotting and help while you wait for the ambulance.
What happens in the ER and early treatment
At the hospital, doctors will confirm a heart attack with ECGs and blood tests. Fast treatment focuses on restoring blood flow. That may mean clot-busting drugs or a procedure like angioplasty and stenting. If you need more information about medications used for heart problems, our pieces on sacubitril and heart failure options and on amlodipine’s role after a heart event are a good next read: Sacubitril vs. Other Medications and Amlodipine: Boosting Heart Attack Recovery.
If someone collapses and is unresponsive, start CPR and use an AED if available. Bystander CPR keeps blood flowing until professionals arrive and dramatically improves survival chances.
After the acute phase, most people leave the hospital with a medication plan—often including antiplatelets, a statin, a beta-blocker or ACE inhibitor, and sometimes newer drugs for specific needs. Medication adherence is one of the biggest factors that reduce the chance of another heart attack.
Recovery also means lifestyle changes. Smoking cessation, a heart-healthy diet, regular walking or cardiac rehab, and managing weight, blood pressure, cholesterol, and diabetes all cut your risk. If swelling or fluid retention is an issue while recovering, a low-sodium plan can help—see our low-sodium tips for practical swaps: Low-Sodium Solutions.
Cardiac rehab programs are underrated. They offer supervised exercise, education, and emotional support—things that speed recovery and lower anxiety. Talk openly with your care team about goals and any fears you have; recovery is physical and mental.
Want to read more? Check patient-focused articles and detailed drug guides in our heart health section. If you have specific symptoms or medication questions, contact your healthcare provider right away—online guides help, but they don’t replace medical care.
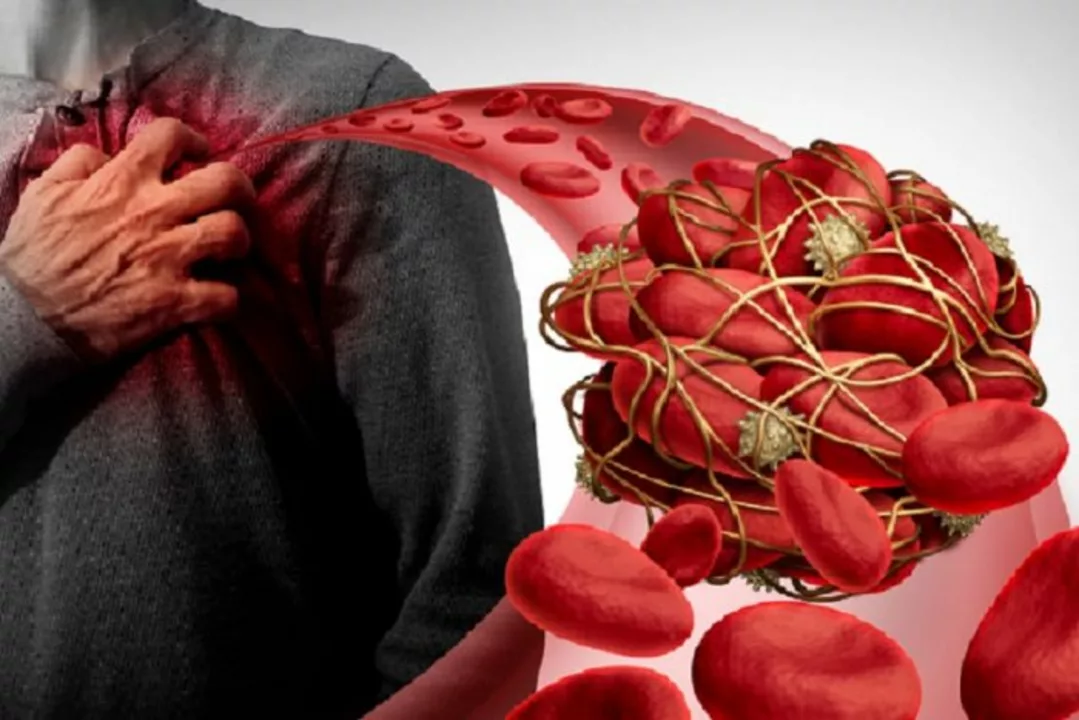
The relationship between blood clots in stents and heart attacks
In a recent study, I came across the relationship between blood clots in stents and heart attacks. It turns out that blood clots formed in stents, which are small mesh tubes used to treat narrow or weak arteries, can lead to heart attacks. This happens when the clot blocks the blood flow in the artery, depriving the heart muscle of oxygen and causing damage. To prevent this, doctors often prescribe blood-thinning medications after stent placement. It's essential for patients with stents to closely follow their doctor's recommendations and attend regular check-ups to minimize the risk of heart attacks.
Read More

