Juvenile Arthritis: What Parents and Teens Really Need to Know
Does your child wake up stiff, limp, or complain about joint pain after school? Those early signs can be juvenile idiopathic arthritis (JIA). It’s not just an "adult" problem — kids get arthritis too, and catching it early makes a big difference. This page gives clear, useful steps: how to spot JIA, what treatments do, and everyday tips to keep life normal.
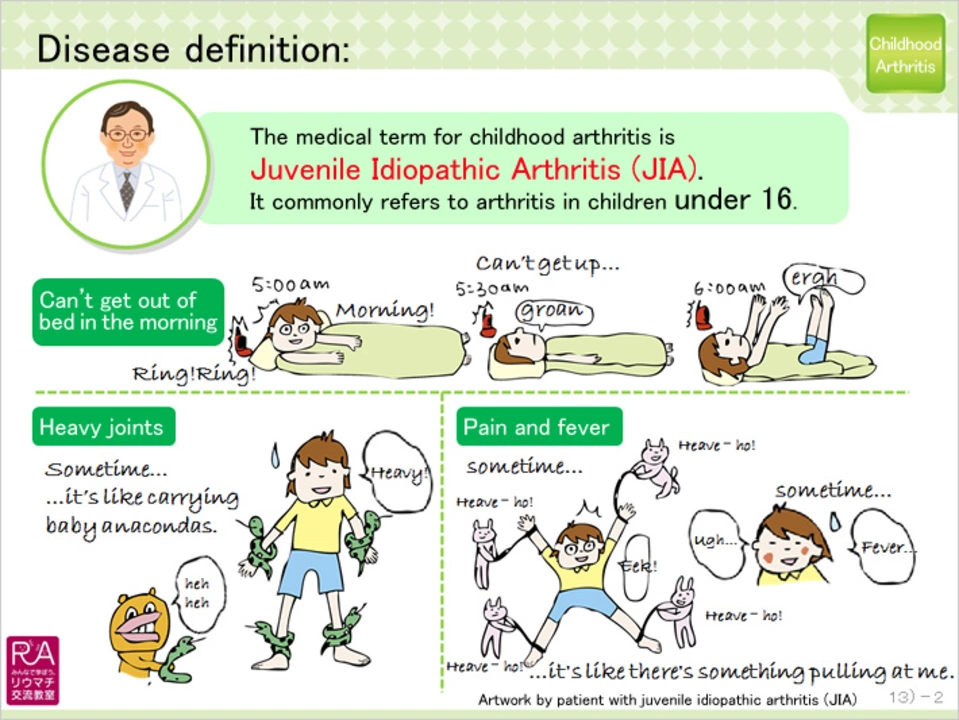
Spotting symptoms and when to see a doctor
Look for swollen, warm, or painful joints that last more than a week. Morning stiffness, limping, unexplained fevers, or a rash with joint pain are red flags. If pain limits play, school, or sleep, make an appointment with your pediatrician and ask for a pediatric rheumatology referral. If a joint is very hot, red, or there’s high fever, get urgent care—septic arthritis needs fast treatment.
Common treatments and what to expect
Treatment aims to reduce pain, prevent joint damage, and keep the child active. Options usually start with NSAIDs (like ibuprofen) for pain control. If pain or inflammation continues, doctors often add a DMARD such as methotrexate to slow disease activity. Biologic drugs (like TNF inhibitors) help when DMARDs aren’t enough. Short courses of steroids can calm severe flares, but long-term steroid use has side effects so doctors try to avoid it.
Medications need monitoring. Expect regular blood tests to check liver function and blood counts, especially with methotrexate and biologics. Ask the team what side effects to watch for and keep a simple chart of dates and symptoms—this helps your clinic spot patterns fast.
Vaccines matter. Kids on many immunosuppressive medicines should avoid live vaccines. Always confirm vaccine timing with the rheumatology or primary care team.
Physical and occupational therapy are part of treatment. PT keeps joints flexible and builds strength; OT teaches safe ways to do schoolwork and sports without extra strain. Heat before activity and cold after can ease pain during flare-ups.
Schools often need a plan. A 504 plan or individualized support can provide rest breaks, extra time between classes, help carrying books, or permission to use elevators. Share doctor notes and simple instructions so teachers know how to help during a flare.
Mental health matters too—chronic pain hits kids emotionally. Watch for mood changes or withdrawal and ask for counseling if needed. Peer support groups or online communities can help teens feel less alone.
Quick practical tips: set a daily med alarm, carry ice packs in a backpack, keep a symptom journal, and involve the child in decisions when they’re old enough. Talk to a pharmacist about drug interactions and safe over-the-counter choices.
If you want resources or links to patient groups, contact your clinic or ask your pharmacist for trusted sites. Early care and a good team make JIA manageable—kids can still do school, sports, and most normal activities with the right plan.
The Different Types of Juvenile Arthritis and Their Characteristics
As a blogger, I recently came across the topic of juvenile arthritis and learned that there are several different types, each with their unique characteristics. The most common form is called Juvenile Idiopathic Arthritis (JIA), which includes subtypes such as oligoarthritis, polyarthritis, and systemic arthritis. Additionally, there's Juvenile Psoriatic Arthritis, which is often related to skin conditions, and Enthesitis-related Arthritis, which affects the areas where tendons and ligaments attach to bones. Knowing the differences between these types of arthritis can help parents and caregivers better understand and manage this challenging condition in children.
Read More